Introduction
Health regulation is complex. If you are new to medico-legal reporting or you have never covered a story involving a complaint about a medical practitioner, it can be challenging getting your head around:
- what the NSW Medical Council does (and does not do)
- how complaints and notifications about individual registered doctors and medical students are dealt with in NSW (compared to other states),
- the work of other organisations which deal with complaints about doctors, such as the NSW Health Care Complaints Commission and the relationship between those organisations and the Council
- the privacy laws which prescribe what a journalist can legally report about when it comes to decisions and conditions imposed on a medical practitioner by the Council and other bodies.
This section of our website includes answers to common media queries and aims to help journalists by providing contextual and background information. We have also included links to other sections of our website for more detailed material on particular topics such as the complaints process and conduct, health and performance pathways.
Journalists seeking information can contact us via the Medical Council’s Communications Unit via email.
What is the Medical Council of NSW?
Our paramount aim is to minimise risk to public health and safety and to maintain acceptable standards of medical practice. The Medical Council of NSW is a regulatory body, established by statute, which receives and manages complaints and notifications about registered medical practitioners in NSW regarding their:
- conduct
- performance, or
- health.
We also manage notifications and complaints about NSW medical students in relation to:
- conduct
- health.
Our powers come from the Health Practitioner Regulation National Law (NSW).
Each complaint we receive is carefully considered in consultation with the NSW Health Care Complaints Commission (HCCC) to assess the nature and extent of any potential risk to one or more patients and to determine appropriate action.
Who is on the Council?
The Council consists of 19 members - 12 are medical practitioners, 6 are non-medical community members and 1 has legal qualifications. Council members are nominated by specialist medical colleges (9), the Health NSW Minister (6), Australian Medical Association (2) and Multicultural NSW (1). One member is nominated jointly by the Universities of Sydney, NSW and Newcastle.
How the Council makes decisions
The Council is funded through a portion of registration fees paid by all doctors in NSW.
Council members are appointed to standing committees which meet monthly to make decisions about individual practitioners being managed within the health, performance and conduct streams.
Council hearings are conducted by delegates of the Council who are selected from a panel of appropriately qualified and experienced community and medical hearing members.
Find out more about our decision-making pathways here.The Council’s secretariat handles the day-to-day work of the Council, includin managing the complaints process and engaing with with both individual complainants and medical practitioners who are the subject of a complaint, coordinating and supporting hearings by the Council and its committees and panels, as well as monitoring doctors who have conditions placed on their registration. Secretariat staff are employed by the NSW Health Professional Councils Authority. They do not have decision-making powers.
Other health regulation organisations
The Australian Health Practitioner Regulation Agency
The Australian Health Practitioner Regulation Agency (Ahpra) is a federal government agency which manages the registration and renewal processes for Australian health practitioners. It publishes a national register for each profession, including details of any public conditions on their registration.
In some states, Ahpra also investigates complaints about doctors and other health practitioners. However, NSW has its own state-based system of investigating and managing complaints against doctors.
NSW Health Care Complaints Commission
The Commission (HCCC) is a an independent health complaints agency that investigates and prosecutes serious complaints about health care in NSW. The Commission deals with complaints concerning the care and treatment provided by health practitioners and health services, including doctors, nurses, pharmacists, dentists, hospitals and other health care providers.
The Commission and the Medical Council work together as co-regulators. A complaint about a doctor or medical student can be made to either organisation. When the complaint is received, the Commission and Council meet to assess whether it should be investigated by the Commission or whether the Council should manage the complaint process.
If it appears a complaint is very serious and could result in a prosecution before the NSW Civil and Administrative Tribunal (NCAT), the Health Care Complaints Commission will be the investigating body.
After an investigation, the Commission may prosecute the most serious complaints in the Tribunal. Cases about medical practitioners are dealt with in the Tribunal’s Health Practitioner Division List in the Occupational Division.
NSW Civil and Administrative Tribunal
The NSW Civil and Administrative Tribunal (NCAT) is a judicial body which adjudicates serious complaints about health professionals. It is independent of the Medical Council and the Health Care Complaints Commission, although the Medical Council nominates medical and community members to sit with the judicial member as a panel on hearings.
The Tribunal has powers to impose conditions on a doctor's registration to keep the public safe, or in the most serious cases, to suspend or cancel their registration for a defined period or indefinitely so the practitioner can no longer practice medicine. The Tribunal may also make a prohibition order preventing a person from providing any health service.
Tribunal decisions about practitioners are published on NSW Caselaw and can also be accessed through the AustLII website.
Complaints and mandatory notifications
Q. What is the difference between a complaint and a mandatory notification?
Anyone may make a complaint about a doctor. However, the law requires health professionals, their employers or educators to notify the Australian Health Practitioner Regulation Agency if they are aware of notifiable conduct in another health professional. Notifiable conduct by a medical practitioner includes practising while intoxicated, sexual misconduct in connection with the practice of medicine, and placing the public at risk of harm. This is called a mandatory notification. A mandatory notification will be assessed in the same way as any other complaint.
Q: How are complaints assessed?
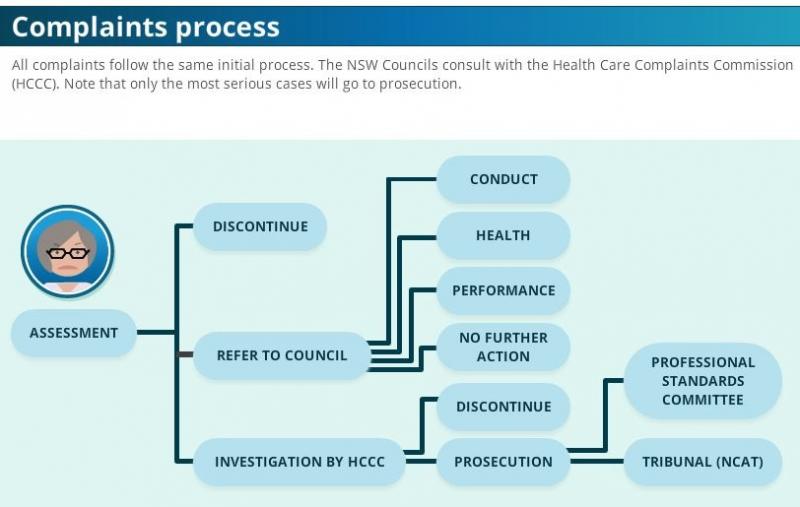
All complaints are assessed in consultation with the Health Care Complaints Commission to determine the appropriate course of action. Most complaints require no further action or are resolved by conciliation.
The most complex or serious complaints are investigated by the Commission and may be prosecuted in the NSW Civil and Administrative Tribunal. Where necessary, the Medical Council may protect the public by suspending a practitioner’s registration pending the outcome of the investigation.
Complaints which raise concerns about the provision of ongoing high standards of care are typically handled by the Medical Council in its conduct, performance or health streams.
Visit the Australian Health Practitioner Regulation Agency to learn how other states assess and manage complaints.
Q: Can I attend hearings?
Some disciplinary hearings (Professional Standards Committees and Tribunal hearings) are generally open to the public and media, unless directed otherwise.
If you attend a hearing, non-publication orders made to protect the privacy of individuals may prevent publication of some details.
Q. Can I get a copy of transcripts from hearings?
Transcripts from hearings by the Medical Council and its committees and panels are not available.
For information about Tribunal hearings, contact the Tribunal.
Q. Why are some matters heard by a Professional Standards Committee and others by the NSW Civil and Administrative Tribunal?
Professional Standards Committees usually hear the less serious allegations of unsatisfactory professional conduct. The Committee exercises quasi judicial authority and may impose conditions on a doctor’s registration. Common conditions include:
- undergoing further training
- having professional mentoring or supervision
- restrictions on a doctor’s working conditions.
The Tribunal adjudicates more serious allegations of professional misconduct which may result in a practitioner’s suspension or deregistration.
Doctors' registration
Q. How do I find out if a doctor is registered?
To check a doctor’s registration, visit the national register of practitioners at the Australian Health Practitioner Regulation Authority (Ahpra).
Q. How do I find out if a doctor has conditions imposed on their registration?
Sometimes a medical practitioner will have conditions placed on their registration. Public conditions relate to how a doctor does their work, such as only being able to work in a supervised environment, having a professional mentor, undertaking further training or not being allowed to perform certain procedures.
Public conditions are published with the practitioner’s registration on the Australian Health Practitioner Regulation Agency’s (AHPRA) national register of practitioners. The Council or the Tribunal may also impose private conditions on a medical practitioner’s registration. Private conditions generally relate to the practitioner's health and are therefore confidential in the same way as is health information about any other member of the community.
Q. What is the difference between suspension and cancellation of a doctor’s registration?
Only the NSW Civil and Administrative Tribunal (NCAT) has the legal power to cancel a medical practitioner’s registration. This might happen following prosecution of a serious complaint which has been investigated by the Health Care Complaints Commission.
The Medical Council can suspend a practitioner’s registration while a complaint is being investigated. This is an interim measure to protect the health and safety of the public while other legal proceedings take place and are decided by a court or tribunal..
Q. What is a Section 150 hearing?
If the Medical Council is concerned that the public may be at risk while a complaint is being assessed, it has the power under Section 150 of the National Health Regulation Law (NSW) to suspend a doctor’s registration or impose conditions on that doctor's registration while the investigation proceeds . Suspension means the doctor may not practice until the suspension is lifted. Only the NSW Civil and Administrative Tribunal can cancel a doctor’s registration.

